In Vitro Fertilisation (IVF) is a medically assisted procreation procedure that reproduces (find something else to do) fertilisation in the laboratory. This fertility technique is offered to patients in order to optimise their chances of pregnancy.
The aim of this treatment is to obtain one or more embryos of optimal quality that can be transferred to the uterus to enable pregnancy to occur.
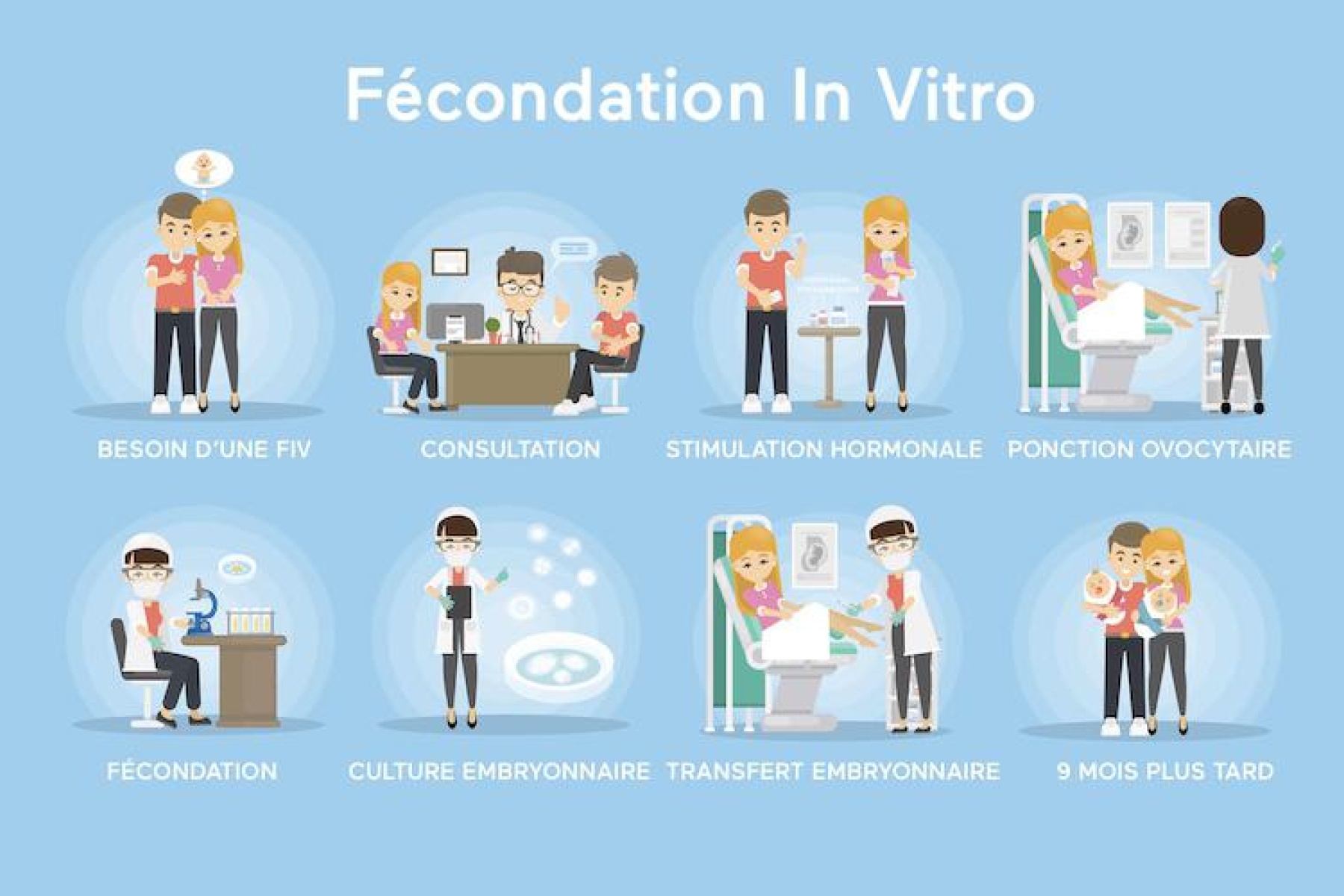
Here are the main stages of IVF:
Ovarian stimulation is the first step in the fertility journey and helps to stimulate ovulation.
After around 14 days, a woman's menstrual cycle produces 1 "dominant" follicle containing 1 mature oocyte, i.e. potentially fertilisable by a spermatozoon.
For in vitro fertilisation, it is necessary to obtain several oocytes in a single cycle after 10 to 15 days of treatment, in order to maximise the chances of obtaining at least 1 transferable embryo.
To achieve this, a hormonal ovarian stimulation treatment using FSH (+/_ combined with LH) is injected under the skin and repeated approximately every 24 hours. You can give these injections yourself at home.
The daily dose prescribed by your doctor is adapted to your particular case and determined by prior assessment criteria such as the count of antral follicles on ultrasound at the start of the cycle and AMH (anti-Müllerian hormone) levels.
Response to ovarian stimulation treatment is assessed by vaginal pelvic ultrasound, combined with hormone levels. This monitoring takes place approximately every 48 hours until an optimum number of mature follicles have reached a size and hormone level indicating the moment of optimal maturity.
During your ovarian stimulation, adjuvant treatments may be offered:
Your doctor will tell you how to monitor these hormone treatments on a daily basis, the results of your tests and the next steps in your treatment via the Wistim monitoring application.
Once you have decided on the optimum moment for maturation, you will need to have an injection of hCG (OVITRELLE®) or Decapeptyl®, which will trigger the final stage of oocyte maturation.
This injection must be given at an extremely precise date and time to allow the subsequent stages to proceed smoothly.
This stage is vital as it enables the gametes (sperm and oocytes) to be supplied to the assisted reproduction laboratory.
On the date determined by your doctor, your partner will collect the sperm (or frozen, self-preserved, or donor sperm, if applicable), which will be used to fertilise the oocytes.
To retrieve the oocytes from the mature follicles, surgery is required. It is performed in an operating theatre, using ultrasound guidance through the vagina, under local or general anaesthetic. Using the ultrasound probe, to which a guide is attached, the doctor pricks each mature follicle on each ovary and a suction system (pump and tube) is used to recover the follicular liquid, which is stored at 37°C and sent to the laboratory.
The laboratory's biologists and technicians will then carry out the actual in vitro fertilisation using your partner's sperm.
The fertility laboratory, which has the gametes of each member of the couple (oocytes for the woman, spermatozoa for the man) will proceed with fertilisation: either by conventional IVF or by IVF ICSI (hyperlink to the article on IVF ICSI) (intra cytoplasmic sperm injection where a selected spermatozoid is microinjected directly into each mature oocyte).
24 hours later, the fertilised oocytes are observed to determine whether fertilisation has occurred and the initial development of the embryos. Embryo culture in vitro (= in the laboratory) can last from 2 to 6 days, and the optimum time for embryo transfer is decided in collaboration between clinicians and biologists.
This is the final stage in your IVF treatment and consists of depositing in the uterus the embryo or embryos that have been selected by the team according to their progress, to give you the best possible chance of pregnancy.
The procedure is painless and is carried out in the gynaecological position during a consultation. It involves inserting a catheter (a flexible plastic tube approximately 1 mm in diameter) into the uterine cavity via the cervix, after fitting a speculum (as for a standard gynaecological examination).
The biologist will have previously placed the embryo(s) in a microdrop of culture medium (liquid) in this catheter. The embryos are not visible to the naked eye. This procedure is painless and can be carried out under ultrasound control.
After the transfer, the catheter is returned to the laboratory, which checks that it is empty. If embryos other than those transferred develop well, the laboratory may freeze them (embryo cryopreservation). This will allow you to benefit from a new embryo transfer without a new puncture.
After the embryo transfer, you will be told when to take the pregnancy test: 14 days after fertilisation, i.e. 14 days after the date of the puncture. This compulsory blood test will determine whether the embryo transfer has progressed favourably and implanted in your endometrium.
This blood test measures the level of beta HCG, a specific hormone produced by the embryo and released into the mother's bloodstream.
Your doctor will tell you how the pregnancy will be monitored.
Adjuvant treatments are necessary for the pregnancy to develop properly: progesterone (vaginal ova, vaginal gel, or subcutaneous injections).